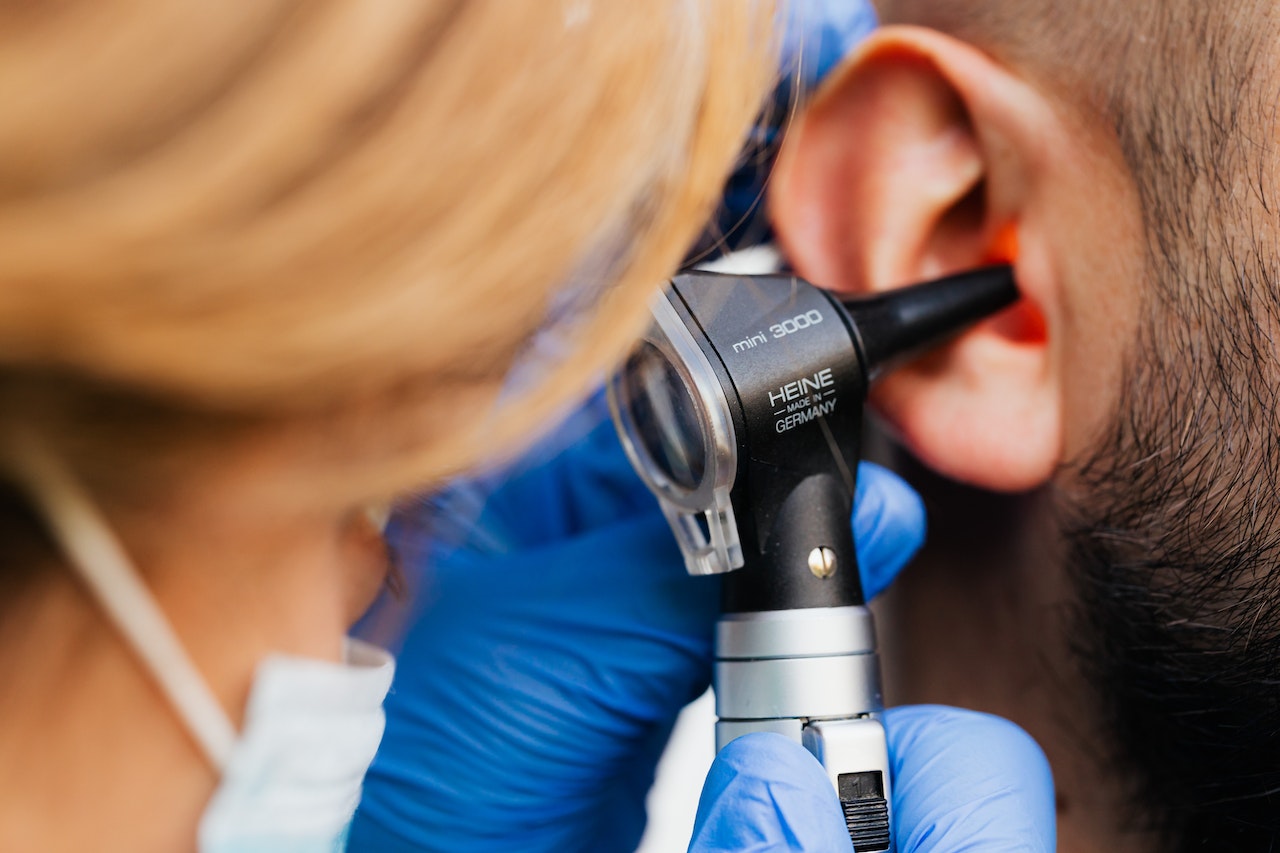
Types of hearing tests
What to expect during your upcoming hearing test.

The 3 key takeaways
- There are different types of hearing tests — Audiologists use different tests to measure the function of different parts of the ear.
- Hearing tests don’t hurt — As long as they’re conducted by a medical professional, hearing tests are completely safe and painless.
- They’re essential for ear health — Get in the habit of getting your hearing tested before you start experiencing problems to catch hearing loss as early as possible.
Feel like your hearing isn’t quite what it used to be? You’re not alone. The World Health Organization estimates more than 1.5 billion people on Earth (20% of the entire population) are affected by deafness and hearing loss.
Fortunately, advancements in modern medicine have made living with most hearing loss disorders manageable. See a professional as soon as you start to notice symptoms of hearing loss, and take a hearing test to gain a better understanding of what’s causing your symptoms.
What is a hearing test?
A hearing test is designed to measure how well a person can hear. Hearing tests help doctors diagnose hearing loss and assess the degree of the patient’s hearing loss.
The testing process usually begins when a primary health provider examines your ears for possible causes of hearing loss, including infection, earwax buildup, and structural abnormalities.
If your provider notices anything unusual in the screening, they may refer you to an audiologist who specializes in ears and hearing for further consultation.
The audiologist will run hearing examination tests, or audiometry tests, by having you put on a special pair of headphones inside a soundproof chamber. Once you’re inside, the doctor will play different tones at different volumes to measure your hearing ability.
The results of these tests are plotted on a graph called an audiogram.
The different types of in-person hearing tests, explained
Most hearing tests are considered sound tests, designed to assess your response to tones or words delivered at different pitches and volumes, or in different noise environments. The tests will help you understand if you need hearing aids or other types of treatment options.
Common types of hearing tests include:
Pure-tone hearing test
Also known as pure tone audiometry, a pure-tone test is one of the first types of hearing tests audiologists will run on patients. After you put on a pair of headphones and sit in a specially designed booth, the doctor will play a series of different sounds at different volumes and pitches to assess how well they travel through your outer and middle ear and into your brain.
Every time you hear a tone, you’ll be asked to raise your hand or press a button. This test helps identify the quietest sounds you can hear at different frequencies, and the results are mapped out on an audiogram.
Bone conduction testing
Bone conduction testing is similar to pure-tone testing but focuses more on the cochlea in the inner ear. The audiologist places a small bone conductor behind your ear that sends tiny vibrations through the bone directly into the inner ear.
That’s why we call this type of testing “bone conduction” as opposed to the traditional air conduction.
Bone conduction testing can also be more accurate in determining the type of hearing loss than traditional air conduction because it bypasses the outer and middle ear, thereby eliminating the effects of obstructions like fluid or earwax buildup.
Speech testing
Speech audiometry involves two different hearing tests: one that measures how loud speech needs to be for you to hear it, and another that measures your ability to distinguish different words when you hear them spoken.
During speech testing, you sit in a sound booth and wear headphones. The doctor plays a recording of several common words spoken at different volumes and asks you to repeat them back to determine your speech reception threshold (SRT), or the minimum hearing level needed for you to be able to understand 50% of the speech you hear.
After this, the audiologist will test your speech discrimination, or word recognition ability.
This test is administered in either a quiet or noisy environment and measures your ability to separate speech from background noise. Both tests take a combined 10 to 15 minutes.
Auditory brainstem response (ABR)
The ABR test helps diagnose abnormalities of the 8th cranial nerve, which contains the nerves that control hearing, balance, and eye movements. To run an ABR test, your audiologist will attach a set of electrodes to your head, scalp, or earlobes.
These electrodes measure your brainwave activity to see how your brain responds to sounds of varying intensities. ABR tests are commonly used to diagnose hearing loss, acoustic tumors, and cerebellopontine angle (CPA) tumors.
They’re also commonly used to screen newborns for hearing problems.
Otoacoustic emissions test (OAEs)
Otoacoustic emissions, or OAEs, are nearly inaudible sounds generated by the vibrating hair cells in the cochlea when soft clicking sounds stimulate them.
This test is run to assess how well the inner ear works. It’s run by inserting a foam or rubber-tipped earphone into the ear, which plays sounds into the canal and measures the sounds that come back.
The test results are produced on a monitor, so you do not need to say or do anything during the test.
The gentle sounds used in OAE tests make them an especially good option for anyone uncomfortable with or unable to complete conventional hearing tests. OAE tests are commonly conducted on toddlers and children who cannot respond to external sounds in a traditional way.
Tympanometry
Tympanometry assesses how well the eardrum moves inside a person’s middle ear. The audiologist places a small probe into the ear with an attachment that changes the pressure on the eardrum by pushing air in and pulling it out. A graph on the device called a tympanogram measures your eardrum’s responses to the pressure and tells the doctor how well it’s working.
Tympanometry tests can determine if your eardrum moves correctly, if it’s too stiff, if it moves too much, or if it’s ruptured.
They’re commonly used to identify conductive hearing loss caused by a buildup of fluid, wax, eardrum injuries, damage to the bones in your inner ear (ossicular damage), or tumors.
Acoustic reflex testing
Acoustic reflex tests are used to assess the condition of a patient’s entire auditory (hearing) system, including the outer, middle, inner ear, and parts of the brainstem related to hearing function.
More specifically, acoustic reflex testing measures the tightening of the stapedial muscle in the middle ear as it responds to loud sounds. This “stapedial reflex,” also called an acoustic reflex, plays a key role in reducing the intensity of loud noises before they can reach the inner ear. Acoustic reflex testing is particularly effective at detecting sensorineural hearing loss, otosclerosis, and non-cancerous tumors known as acoustic neuroma.
This type of hearing test is non-invasive, requiring only headphones and a small probe placed in the ear canal. Sounds of varying intensities are played through the headphones and used to measure the ear’s reflex responses.
Audiologists commonly perform a standard hearing test before acoustic reflex testing to get a sense of a patient’s baseline hearing levels going into the exam.
Weber hearing test
Commonly referred to as a “tuning fork test,” Weber hearing tests are quick, easy to perform, and require relatively little equipment compared to more complicated hearing tests. That’s why audiologists commonly employ this type of testing first when determining the cause of a patient’s hearing loss.
Carried out in a quiet room for accuracy, a Weber test consists of the doctor striking a tuning fork and placing it against the middle of a patient’s head. The resulting vibrations are carried through the skull before reaching the cochlea (a fluid-filled, spiral-shaped cavity) in the inner ear. The patient then indicates where they’re able to best hear the sound: in their left ear, right ear, or equally between both ears.
Audiologists commonly perform Weber tests alongside another type of tuning fork test called Rinne testing when screening for conductive and sensorineural hearing loss.
While the Weber test is useful for identifying which ear is affected by hearing loss, the Rinne test measures how well a patient can hear sounds conducted through air versus sounds conducted through the bones of the ear.
Used together, these two tuning fork tests give audiologists an effective way to pinpoint the location and cause of a patient’s hearing loss.
Online hearing tests, explained
If you suspect you might be suffering from hearing loss but don’t have access to in-person care, an online hearing test is a quick, easy way to gain a better understanding of your condition. Many online tests are free to take, and they can be completed in just a few minutes from the comfort of your own home.
To take an online hearing test, patients put on a pair of headphones and listen to sounds at different volumes and frequencies. The test’s software records your results as you go and offers custom feedback at the end of the test based on your perceived hearing ability.
👉 Check out our guide to online hearing tests for in-depth info on the most popular online tests available today.
Who needs a hearing test?
The simple answer? Everyone. Hearing tests are recommended once every 3 to 5 years for healthy adults and even more frequently for newborn babies, children, older adults, and anyone experiencing symptoms of hearing loss.
- Newborn babies. Newborns should have their hearing checked before they’re one month old. This procedure is safe, painless, and typically only lasts a few minutes. Some hospitals may even conduct an initial screening while the baby is still in the hospital. Take your newborn to see an audiologist if they don’t pass their initial hearing screening.
- School-age children. Kids should have regular hearing check-ups as their bodies develop. Screening tests are commonly performed at ages 4, 5, 6, 8, 10, and later again in the preteen and teenage years.
- Adults experiencing hearing loss. Get your hearing checked as soon as you suspect you might be suffering from hearing loss or once a year after age 55.
Symptoms include difficulty understanding what others are saying, especially in noisy environments; frequently asking others to repeat themselves; trouble hearing high-pitched sounds; a ringing in your ears known as tinnitus; and regularly playing the TV or music louder than others find comfortable.
Getting your results and next steps
Once the appropriate hearing tests have been run, your audiologist will use the test results to diagnose the type of hearing loss you have (if any) and provide you with treatment options.
Pure-tone testing results. Pure-tone testing results are plotted out on an audiogram, a graph that displays the frequencies a patient can hear at different intensities. The results of these tests allow doctors to calculate a patient’s pure-tone threshold (PTT), a term used to describe the softest sound an individual can hear in decibels (dB).
- Patients with a PTT between 0 and 25 dB are said to have normal hearing, while numbers above this range indicate differing degrees of hearing loss.
- Mild hearing loss is defined by a PTT between 26 and 40 dB.
- Moderate hearing loss is between 41 and 55 dB.
- Moderate-severe hearing loss is between 56 and 70 dB.
- Severe hearing loss is between 71 and 90 dB.
- Profound hearing loss is anything above 90 dB.
Inner ear testing results. Results from inner ear tests like bone conduction testing are generally used to expand on the results of a traditional pure-tone test. If results from these two tests are the same or similar, a patient is said to have sensorineural hearing loss. On the other hand, if the tests yield varying results, the patient may be suffering from conductive hearing loss.
Middle ear testing results. Middle ear tests like tympanometry and acoustic reflex testing record the movement of the bones and other small muscles in the middle ear. Tympanometry results are plotted on a tympanogram, which will show the audiologist if your eardrum is moving correctly, moves too much or too little, or has a hole in it.
Speech testing results. Much like pure-tone testing, speech testing results are mapped out on a speech audiogram. Patients are evaluated for their speech recognition threshold (SRT), which indicates the lowest level at which they can hear certain words, and a word recognition score (WRS), which measures the number of words they can hear correctly at an SRT of 30 dB. Scores between 85 and 100 percent are considered normal, with the number decreasing as a patient’s degree of hearing loss increases.
Otoacoustic testing results. Tests like otoacoustic emissions (OAEs) gauge the inner ear’s response to sound by measuring small sounds generated by the cochlea in response to external stimuli. If OAEs are present in the cochlea, a patient is said to have normal or near-normal hearing. The absence of OAEs is more concerning, as it could indicate hearing loss, wax or fluid buildup, infection in the middle ear, or a malformed inner ear.
Acoustic reflex testing results. Acoustic reflex results will show the threshold levels at which a patient’s stapedial reflex is triggered and if there are any abnormalities in the reaction time.
Weber and Rinner testing results. Weber and Rinne tests are used to diagnose cases of unilateral hearing loss, and distinguish cases of sensorineural hearing loss from conductive hearing loss. A person is considered to have normal hearing if they hear the sounds of a Weber test equally in both ears, while healthy Rinne test results will show a patient’s air conduction is better than bone conduction.
Types of hearing loss
Just like hearing loss can be caused by different factors, there are also different types of hearing loss. These include:
- Sensorineural hearing loss. Also referred to as “nerve deafness,” this type of hearing loss occurs when there’s damage to the tiny hair cells inside the inner ear, or the neural pathways connecting the ears to the brain. Sensorineural hearing loss is the most common type of hearing loss. It’s a permanent condition in most cases, with symptoms ranging from mild to profound.
- Conductive hearing loss. This type of hearing loss occurs when sounds cannot get through the outer and middle ear. These are commonly caused by obstructions like fluid buildup from colds or allergies, earwax, or benign growths in the ear. People with conductive hearing loss may have difficulty hearing soft sounds, or hear louder sounds as muffled.
- Mixed hearing loss. As its name suggests, conductive hearing loss is used to describe cases in which a person suffers from both sensorineural and conductive hearing loss.
- Auditory Neuropathy Spectrum Disorder (ANSD). ANSD is a rare disorder in which the ear can still pick up sounds and send signals to the brain, but it sometimes scrambles the signals in a way that prevents the brain from properly interpreting them. ANSD is usually caused by damage to the auditory nerve, which connects the cochlea in the inner ear to the brain. Many people with ANSD are also born with it.
Treatment options
Treatment will vary depending on the type of hearing loss. Cases of sensorineural hearing loss are commonly treated with hearing aids, electronic devices worn in or behind the ear to amplify sounds and make speech more understandable.
There are many different types of hearing aids — read our audiologists’ advice on how to choose a hearing aid.
People with mild to moderate hearing loss can also benefit from assistive listening devices like personal amplifiers, amplified telephones, and TV listening sets.
Severe cases of sensorineural hearing loss may require a cochlear implant, a device that bypasses a heavily-damaged inner ear and sends electrical impulses to the auditory nerve in its place.
Because cochlear implants are surgically implanted, you must undergo a thorough evaluation by an audiologist to make sure you’re a suitable candidate.
Cases of conductive hearing loss can usually be treated by removing the obstruction causing the problem. This can be as simple as removing an earwax impaction or foreign body, though sometimes medical intervention is required in the form of surgery or pressure equalization (PE) tubes.
Hearing aids and assistive listening devices can also benefit people suffering from conductive and mixed hearing loss.
👉 See an audiologist for a comprehensive treatment plan that accounts for the specifics of your hearing loss.
Going in for a hearing test can be an uncomfortable experience, but understanding how and why they’re conducted can help ease your concerns. Regular check-ups are the best way to ensure healthy hearing and prevent any serious problems from developing in the future.
Why trust audiologists.org
All content in this article was reviewed for scientific accuracy by Jessica Hinson Au.D, who obtained her Doctor of Audiology degree from the University of South Alabama. She is licensed in the state of Alabama, where she practices in a multi-physician ENT office. Dr. Hinson specializes in adult and pediatric hearing exams, hearing aids, diagnosis and treatment of balance disorders, and auditory electrophysiology.
Frequently asked questions
What is the most common hearing test?
When patients go in for hearing loss, the first test most audiologists will run is an otoscopy test. An otoscope is a handheld tool equipped with light and magnification that allows your audiologist to check for wax buildup and other abnormalities. Aside from this, pure-tone testing is considered the most common type of hearing test.
Which hearing test is most accurate?
There’s no “one size fits all” test when it comes to hearing loss, but the most accurate way to evaluate your hearing is always by scheduling an in-person appointment with a professional audiologist. They’ll be able to give you valuable information regarding your type of hearing loss and treatment options.
What is the difference between a hearing screening and a hearing evaluation?
A hearing screening is a quick test to check your hearing that you either pass or fail. On the other hand, a hearing evaluation is a comprehensive examination performed by a licensed audiologist or hearing specialist. This includes a review of your full case history and multiple types of hearing tests.
Will I need to do anything to prepare for a hearing test?
No. Unless specified by your audiologist, no special preparations are required for any kind of hearing test.
Is an audiologist better than an ENT?
No doctor is “better” than the other. An audiologist can help you manage the symptoms of hearing loss, while an ENT doctor provides treatments and surgery to resolve medical issues. Both are invaluable in keeping our hearing healthy.
This article was updated on 4/9/2024. Our team added new information on other common hearing tests and what to expect from hearing test results. This article was originally published on 5/1/2023.